Acute Respiratory Distress Syndrome
Acute respiratory distress syndrome (ARDS), also known as respiratory distress syndrome, adult respiratory distress syndrome, shock lung, or wet lung, is a severe form of respiratory failure characterised by rapid onset of widespread inflammation in the lungs. It can significantly impair the lungs' ability to exchange oxygen and carbon dioxide, leading to a high mortality rate ranging from 35% to 50%.

Signs and Symptoms
The onset of ARDS typically occurs within a week of an inciting event, although symptoms can appear as early as two hours afterward. Symptoms include shortness of breath (dyspnea), rapid breathing (tachypnea), bluish skin coloration (cyanosis), muscle fatigue, general weakness, low blood pressure, a dry hacking cough, and fever.
Complications
Complications of ARDS can be severe and include:
- Lungs: Barotrauma, pulmonary embolism (PE), pulmonary fibrosis, ventilator-associated pneumonia (VAP).
- Gastrointestinal: Bleeding, dysmotility, pneumoperitoneum, bacterial translocation.
- Neurological: Hypoxic brain damage.
- Cardiac: Abnormal heart rhythms, myocardial dysfunction.
- Kidney: Acute kidney failure, positive fluid balance.
- Mechanical: Vascular injury, pneumothorax from pulmonary artery catheter placement, tracheal injury or stenosis from intubation.
- Nutritional: Malnutrition, electrolyte abnormalities.
Other notable complications include failure of multiple organs, pulmonary hypertension, and complications from prolonged hospitalisation such as blood clots, stress ulcers, and mental health issues.
Causes
ARDS can result from both direct and indirect lung injuries. Direct causes include pneumonia (bacterial and viral), aspiration, inhalational lung injury, lung contusion, chest trauma, and near-drowning. Indirect causes include sepsis, pancreatitis, trauma, cardiopulmonary bypass, transfusion-related acute lung injury (TRALI), burns, and increased intracranial pressure.
Pathophysiology

ARDS is characterised by fluid accumulation in the lungs not explained by heart failure, termed noncardiogenic pulmonary oedema. The condition usually follows an acute injury to the lungs, causing flooding of the alveoli, atelectasis, and hypoxaemia. The most common histopathological finding in ARDS is diffuse alveolar damage (DAD), marked by inflammation and hyaline membrane formation in alveolar walls.
Diagnosis
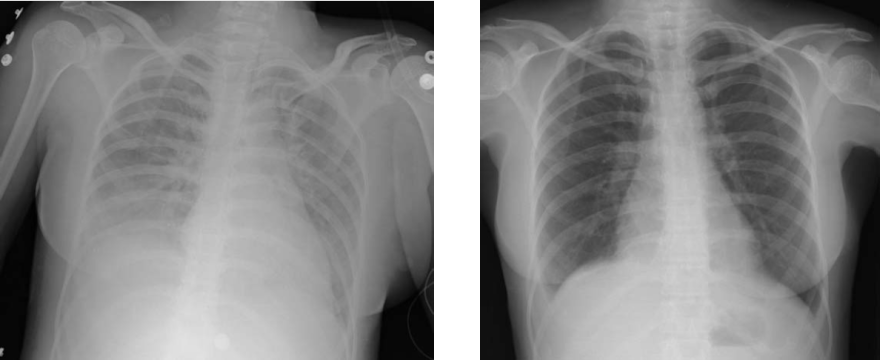
According to the Berlin definition (2012), ARDS is diagnosed when there is acute onset within one week of a known clinical insult, bilateral opacities on chest imaging, and respiratory failure not explained by heart failure or volume overload. The severity is graded based on the PaO2/FiO2 ratio:
- Mild: 201-300 mmHg
- Moderate: 101-200 mmHg
- Severe: ≤ 100 mmHg
Treatment
The primary treatment for ARDS involves mechanical ventilation, aimed at maintaining acceptable gas exchange and minimising lung injury. Ventilation strategies include using low tidal volumes (6 ml/kg) to reduce volutrauma and employing positive end-expiratory pressure (PEEP) to recruit collapsed alveoli.
Mechanical Ventilation
Mechanical ventilation is often delivered through endotracheal intubation or tracheostomy. Low tidal volume ventilation has been shown to improve survival rates. Airway pressure release ventilation (APRV) and PEEP are also used to enhance oxygenation and prevent alveolar collapse.
Prone Position
Repositioning patients into the prone position can improve oxygenation by relieving atelectasis and enhancing perfusion. Early prone positioning has been shown to confer a significant mortality benefit in severe ARDS cases.
Fluid Management
Managing fluid balance through diuresis or fluid restriction can improve pulmonary function and outcomes.
Medications
The use of corticosteroids, such as dexamethasone, may improve ventilator-free days, though their impact on overall survival is uncertain. Inhaled nitric oxide can enhance oxygenation but does not improve survival rates.
Extracorporeal Membrane Oxygenation (ECMO)
ECMO can be considered for patients with severe ARDS unresponsive to conventional treatment, offering an alternative means of gas exchange and reducing the need for high-pressure ventilation.
Prognosis
The prognosis for ARDS remains poor, with a mortality rate of approximately 40%. Survivors often experience long-term physical and psychological sequelae, including exercise limitations and decreased quality of life.
Epidemiology
ARDS affects about 3 million people globally each year. The most common triggers include pneumonia, sepsis, and trauma. The incidence increased during the COVID-19 pandemic due to the virus's impact on respiratory function.
Self-assessment MCQs (single best answer)
Which of the following is a hallmark feature of ARDS?
ARDS is most commonly associated with which of the following conditions?
The Berlin definition is used to diagnose ARDS. Which of the following is NOT a criterion in the Berlin definition?
Which of the following is a common histopathological finding in ARDS?
What is the primary treatment strategy for ARDS?
Which of the following complications is NOT typically associated with ARDS?
The use of low tidal volumes in mechanical ventilation for ARDS patients is primarily aimed at:
Which positional strategy has been shown to improve oxygenation in severe ARDS cases?
What is the approximate mortality rate associated with ARDS?
Which of the following can be considered for patients with severe ARDS unresponsive to conventional treatment?
Dentaljuce
Dentaljuce provides Enhanced Continuing Professional Development (CPD) with GDC-approved Certificates for dental professionals worldwide.
Founded in 2009 by the award-winning Masters team from the School of Dentistry at the University of Birmingham, Dentaljuce has established itself as the leading platform for online CPD.
With over 100 high-quality online courses available for a single annual membership fee, Dentaljuce offers comprehensive e-learning designed for busy dental professionals.
The courses cover a complete range of topics, from clinical skills to patient communication, and are suitable for dentists, nurses, hygienists, therapists, students, and practice managers.
Dentaljuce features Dr. Aiden, a dentally trained AI-powered personal tutor available 24/7 to assist with queries and provide guidance through complex topics, enhancing the learning experience.
Check out our range of courses, or sign up now!


