Ulcerative Colitis
Ulcerative colitis (UC) is a type of inflammatory bowel disease (IBD) that primarily affects the colon and rectum. It is characterised by long-term inflammation and ulcers in the lining of the colon.
The condition often presents with periods of active disease (flares) and times of remission.
Signs and Symptoms
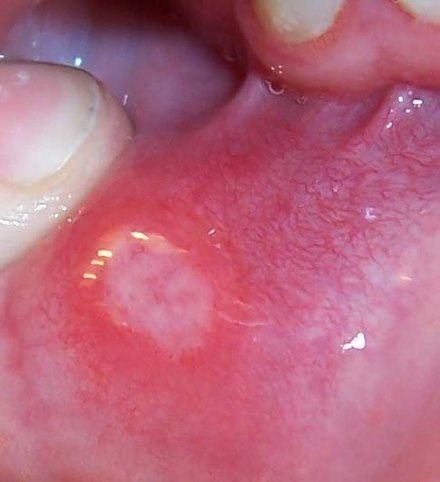
The primary symptoms of UC include abdominal pain and diarrhoea mixed with blood (hematochezia). Other common symptoms are weight loss, fever, anaemia, dehydration, loss of appetite, fatigue, sores on the skin, urgency to defecate, and rectal pain.
During active disease phases, patients may experience frequent, bloody stools and significant discomfort.
Gastrointestinal Symptoms
People with UC typically have diarrhoea with blood, rectal urgency, and abdominal pain. Severity can range from mild discomfort to severe pain.
Chronic bleeding from the gastrointestinal tract can lead to anaemia. The extent of inflammation can vary, affecting only the rectum (proctitis), the left side of the colon, or the entire colon (pancolitis).

Extraintestinal Symptoms
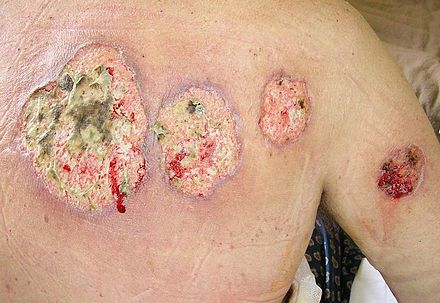
UC can also cause symptoms outside the gastrointestinal tract, affecting the eyes, skin, and joints. Common extraintestinal manifestations include uveitis, erythema nodosum, and arthritis.
Complications such as primary sclerosing cholangitis (PSC) can occur, leading to liver disease.
Diagnosis
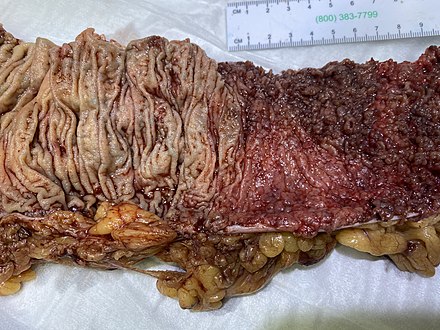
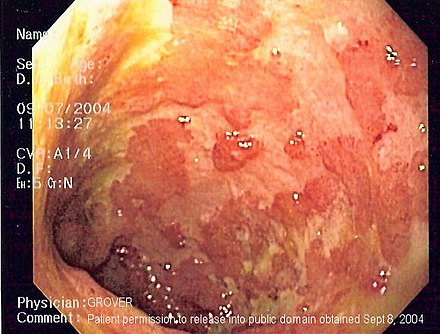
UC is diagnosed primarily through colonoscopy with tissue biopsies. Endoscopic examination reveals continuous areas of inflammation starting from the rectum.
Laboratory tests can show anaemia, elevated inflammatory markers (CRP and ESR), and stool tests help rule out infections.


Treatment
Treatment for UC aims to induce and maintain remission. Medications include aminosalicylates (e.g., mesalazine), corticosteroids for acute flares, immunosuppressants (e.g., azathioprine), and biological agents (e.g., infliximab).
Severe cases may require surgery, such as colectomy, which can be curative for colonic disease.
Medications
First-line maintenance therapy often involves mesalazine. Corticosteroids are used for short-term relief during active flares.
In more severe cases, immunosuppressants and biologic agents are necessary to control the disease.
Surgery
Surgical options include proctocolectomy with ileostomy or ileal pouch-anal anastomosis (IPAA). Surgery is typically reserved for patients who do not respond to medical treatment or develop complications like colon cancer.
Prognosis
The prognosis for UC varies. Some patients experience mild symptoms, while others may have severe disease requiring surgery.
Long-term management is focused on maintaining remission and monitoring for complications, such as colorectal cancer, which has an increased risk after ten years of disease duration. Regular colonoscopies are recommended for surveillance.
Self-assessment MCQs (single best answer)
Which part of the gastrointestinal tract is most commonly affected by ulcerative colitis?
What is a common extraintestinal manifestation of ulcerative colitis?
Which of the following is NOT a typical symptom of ulcerative colitis?
What is the first-line maintenance medication for ulcerative colitis in remission?
Which of the following complications is commonly associated with severe ulcerative colitis?
What is the recommended treatment for inducing remission in moderate to severe ulcerative colitis?
Which laboratory marker is commonly elevated in patients with active ulcerative colitis?
What is the characteristic endoscopic finding in ulcerative colitis?
Which genetic factor is associated with an increased risk of developing ulcerative colitis?
What is a potential long-term complication of chronic ulcerative colitis?
Dentaljuce
Dentaljuce provides Enhanced Continuing Professional Development (CPD) with GDC-approved Certificates for dental professionals worldwide.
Founded in 2009 by the award-winning Masters team from the School of Dentistry at the University of Birmingham, Dentaljuce has established itself as the leading platform for online CPD.
With over 100 high-quality online courses available for a single annual membership fee, Dentaljuce offers comprehensive e-learning designed for busy dental professionals.
The courses cover a complete range of topics, from clinical skills to patient communication, and are suitable for dentists, nurses, hygienists, therapists, students, and practice managers.
Dentaljuce features Dr. Aiden, a dentally trained AI-powered personal tutor available 24/7 to assist with queries and provide guidance through complex topics, enhancing the learning experience.
Check out our range of courses, or sign up now!


